

People with excessive sweating live with a variety of day-to-day challenges: personal and professional limitations, ongoing discomfort, embarrassment, other emotional burdens, and more.
We are, however, seeing great improvements in hyperhidrosis treatment and in the understanding of this often under-acknowledged condition. Yet we still hear from hyperhidrosis patients about difficult, serious and often irreversible side effects caused by endoscopic thoracic sympathectomy (ETS) surgery.
After all other treatments have been tried, adjusted for individual circumstances, combined in nuanced fashion, and still found to be ineffective, surgical treatment for excessive sweating may be an option but should be considered carefully. There are a few different types of surgery that may be used to treat hyperhidrosis. The most invasive of these is endoscopic thoracic sympathectomy (ETS). ETS is considered a last resort because it frequently causes serious, irreversible compensatory sweating (excessive sweating on large areas of the body or all over) as well as other debilitating effects such as extreme hypotension (low blood pressure), arrhythmia (heart rhythm issues), and heat intolerance. Most practitioners do not recommend ETS surgery because of the serious negative side effects of the procedure. Of note, while ETS was first performed in Sweden, it is now outlawed in that country due to its side effects.
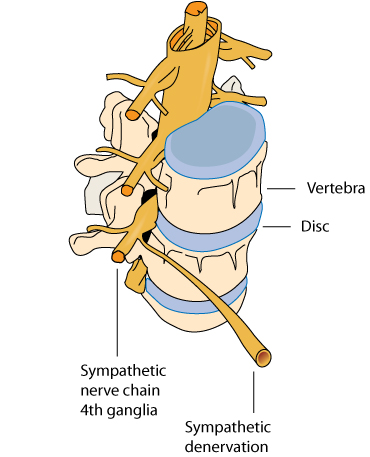
During ETS surgery, surgeons attempt to interrupt the transmission of nerve signals from the spinal column to the sweat glands and to thus prevent these nerve signals from "turning on" the sweat glands.
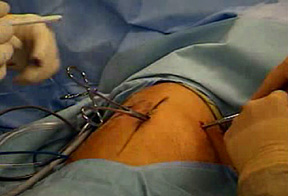
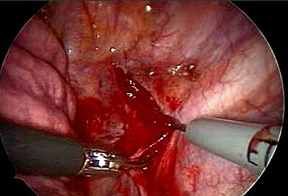
The procedure is performed with the patient under general anesthesia. A miniature camera is inserted into the chest under the armpit. A lung is temporarily collapsed so the surgeons can cut or otherwise destroy the nerve paths associated with the overactive sweat glands. This procedure is permanent; there have been no successful reversal procedures reported.
After the surgeon completes this procedure on one side of the body, he/she performs the same procedure on the other side. ETS is most often used to treat severely sweaty palms, sometimes the combination of sweaty palms and sweaty underarms, and rarely facial flushing and sweating, but it is a major surgery (even though it's sometimes termed 'minimally invasive') with significant risks and limited success.
An article in a British newspaper described the case of a young woman, 27-year-old Louise Field, who became brain damaged after suffering from a lack of oxygen when her lung was accidentally punctured during ETS surgery to control her palmar hyperhidrosis. With no chance of recovery, her parents Patricia and Phillip Green made the heartbreaking decision to turn off Louise's life support machine two days after the procedure.
Louise Field's death is an extreme case, with clear indications of negligence on the part of her medical team, but it serves as a cautionary tale for those who are considering ETS for their excessive palmar sweating. Because ETS surgery has several serious side effects, and because its results are largely irreversible, many experts consider it an option of last resort.
Compensatory sweating is excessive sweating that occurs on the back, chest, abdomen, legs, face, and/or buttocks as a result of ETS surgery. It can be equally or even more extreme than the original sweating problem. In a study involving 121 patients at the Medical City Hospital of Dallas, Texas, compensatory sweating occurred in more than 80% of the patients undergoing ETS. Similarly, in a Danish study conducted at the Aarhus University Hospital, 90% of the patients undergoing ETS for underarm sweating, reported compensatory sweating, half of whom were forced to change their clothes during the day because of it.
Compensatory sweating is very difficult to treat and is a "huge challenge" say members of our Board of Directors. Oral medications can be used, with other treatments, to make it it "a little better," they say, but even with multiple therapies, "we can't get patients with compensatory sweating back to where they were before and it may take a lot of therapies to get results."
"None of my patients have had this procedure--probably because I do not recommend ETS very often and I never recommend lumbar ETS for plantar hyperhidrosis. I have known of too many patients with severe complications, especially debilitating compensatory sweating, following routine ETS surgery for palmar hyperhidrosis. I advise other physicians against such procedures, especially the lumbar type. ETS for palmar hyperhidrosis is a procedure I might approve as an absolute last resort, especially if performed by a competent surgeon. This procedure has a very high success rate but also a very high rate of compensatory sweating." -- Daniel A. Carrasco, MD Austin, TX
The account below from a patient experiencing a high degree of compensatory sweating, shows the downside of this procedure.
"I am a 38-year-old woman who feels totally out of place. I started off sweating on my hands and feet and I had the ETS surgery. Immediately after the surgery, while I was still in the hospital bed, I awakened to a sweaty butt, back, and legs. The doctor said it was compensatory sweating and it has been more than 4 years and in that time I have totally removed myself from everyone. I have had to switch job positions two times. I can't speak or stand up in front of a crowd. My clothes get soaked. People often say I have a stain on my butt. My back, chest, and stomach constantly sweat. My ex-boyfriend called me "sweaty butt" and always made comments about the bed being wet. I wear a lot of black and have spent hundreds of dollars on Under Armor gear and underarm pads. Nothing works. I thought it would go away. I continued to sweat and eventually, I requested the clamps used to block the nerves be removed. The doctor stated the nerve should regenerate itself and the compensatory sweating would stop and my hands and feet would probably continue to sweat.
This condition causes me great depression. I cannot wear shorts, tank tops, or light-colored shirts. My jeans get wet in the butt and around the waist. I don't date.
Every time I do, the young men always ask me 'What is wrong?' and 'Why are your clothes wet? It's disgusting.' I cry and cover up a lot. I need help."
We strongly encourage people who are considering this procedure to do their homework; research all hyperhidrosis treatment options and talk to dermatologists and/or other healthcare professionals who are well versed in the techniques and side effects of this surgery. It's also important to talk to other patients who've had the surgery to get feedback on both their surgeons and their results.
Dr. James Headrick, a thoracic surgeon who performs ETS surgery for palmar hyperhidrosis in Chattanooga, TN, says that surgeons must take great care to "focus on optimum patient selection." He adds, "It is really just a matter of trying to limit the procedure to those with severe primary PALMAR hyperhidrosis who have failed all other reasonable options. There is also focused attention on the level of nerve to cut in order to try to minimize compensatory sweating. The procedure is now down to a single 3-5 mm single incision in each axilla, with no sutures used; it's an outpatient procedure with a 3-5 day recovery." He concludes by saying, "all patients have to be willing to accept some degree of compensatory sweating."
In short: if you or someone you care about is considering ETS, serious caution and significant research should accompany the decision. Stop by our Clinician Finder directory too; look up healthcare specialists in your area who offer hyperhidrosis treatment. It is recommended that you talk to a dermatologist before resorting to surgery. A dermatology team may be able to recommend effective non-surgical options and may recommend and be able to perform a local surgery as opposed to ETS.
Before considering ETS surgery, patients and their clinicians should be confident that they have thoroughly exhausted all other available treatment options (as appropriate depending on the area of sweating), including clinical strength antiperspirants, Botox injections, Brella*, iontophoresis, iontophoresis with the addition of an anticholinergic, miraDry, oral medications to treat hyperhidrosis, Qbrexza, Sofdra, and appropriate combinations of these treatments. (*Please note that as of June 2025, Candesant Biomedical, the company behind Brella, is in the process of being sold. As a result, access to Brella is currently limited and may only be available through clinics that already have it in their inventory.)
Keep in mind that surgical procedures for the treatment of excessive sweating are considered major surgery and require special training. If you are considering surgical treatment, be sure your surgeon is well-trained and informed of the most recent research. When considering a surgeon, ask about the percentage of their patients who experience side effects such as compensatory sweating with ETS, and demand to speak to a variety of patients he/she treated for hyperhidrosis. Since some complications from this surgery become apparent years after the procedure, you should speak with patients who had the operation at least two years ago. Ask these patients about their satisfaction with this surgery, whether they are experiencing side effects, and whether they would recommend surgery to others.
When researching ETS, be certain to review peer-reviewed, published studies. Simply typing "ETS" into Google will bring up a bevy of misleading information. The Internet is loaded with bogus claims about ETS and hyperhidrosis treatments. This is one reason why so many people who've undergone ETS are left devastated by the side effects. To learn more about the common complications of ETS, read Internet message boards discussing the procedure and its aftereffects.
Now as never before, people with hyperhidrosis have options. Talk to an expert and find the best choice for you. Get started today!
Latest Blogs